Intramuscular Haemangioma of Vastus Lateralis Presenting as Stiffness of Knee in an Adolescent.
Iftikhar H Wani1, Muneer Farooq1, A R Budoo1
1Hospital For Bone And Joint Surgery Barzulla Srinagar Jammu And Kashmir India. 190005
Address of Correspondence
Dr Iftikhar H Wani
Hospital For Bone And Joint Surgery Barzulla Srinagar Jammu And Kashmir India. 190005
Email: drihwani@yahoo.co.in
Abstract
Objective: Intramuscular haemangiomas may present later in life as a cause of persistent symptoms and is frequently misdiagnosed, leading to a diagnostic delay of many years. Non specific presentation like knee stiffness is very rare and is not reported yet in the literature.
Case presentation: We present a case of an atypical presentation of intramuscular haemangioma as stiffnes of knee in a 16 year old boy with a diagnostic delay of 2 years.
Conclusion: Intramuscular haemangioma should be considered in the differential diagnosis of unexplained stiffness of the nearby joint and should be evaluated early to prevent diagnostic delay and achieve good results.
Key Words: ????
Introduction
Haemangiomas are common benign soft tissue tumours, comprising 7–10% of all soft tissue tumours1.Cutaneous haemangiomas, the most common1, are usually found in childhood. Intramuscular haemangiomas make up 0.8% of all haemangiomas 2. Intramuscular haemangiomas may present later in life as a cause of persistent symptoms3 . Nonspecific presentations are also common and may lead to a diagnostic delay of many years4. Magnetic resonance imaging is the investigation of choice. Intramuscular haemangioma should be considered in the differential diagnosis of unexplained pain and swelling in a muscle3. We present the case of an atypical presentation of intramuscular haemangioma of the vastus lateralis as knee stiffness. Treatment methods have varied in the past. Angiography can help to find some feeder vessels and embolisation can be done in the same session. In the absence of specific vessels to embolise, complete surgical excision, is the treatment of choice.
Case Presentation
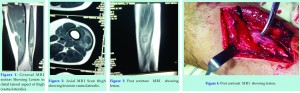
A 16 year old boy presented with stiffness of the left knee. It was most noticeable when he was going upstairs and running. The symptoms had been present for about two years. Patient complains of occasional pain around knee while running or sporting activities. There was a small tender swelling on the outer aspect of distal third of thigh. The swelling becomes prominent on forcefull contraction of quadriceps. The knee range of motion was only 0-90˚. There was no history of major trauma, instability, or locking. His other medical history was unremarkable. There was pain with resisted quadriceps contraction, no effusion, and ligament testing was stable. There were no signs of patellofemoral irritability. The differential diagnosis included suprapatellar bursitis, quadriceps tendinopathy, synovial dysplasia, and extraarticular soft tissue tumour. The patient was advised to present for an x ray examination and Magnetic resonance imaging of the left thigh and knee. The radiographic results were unremarkable. MRI shows areas of altered intensity which were hyperintense on T1w and T2w sequences with inhomogenous enhancement on post contrast studies on lateral aspect of thigh (vastus lateralis)( Fig.1,Fig.2, Fig.3).
The patient was referred to a vascular surgeon whose opinion was that the lesion was too big to excise. The patient was then planned for surgical excision of the lesion. Intraoperatively there was a big lesion involving vastus lateralis. Grossly the distented vessels were seen crossing the lesion. It was bluish in colour and about 4cm ˣ 3cm in size ( Fig.4).
Complete excision of lesion was done. Hemostasis was achieved and fluffy cotton and bandage dressing was applied. Postoperative period was uneventfull and knee range of motion exercises was started. After 6 months of follow up knee is free with range of motion from 0-110˚.
Discussion
Hemangiomas of bone constitute 1% of all primary bone tumours. The soft tissue types are even less common and often arise in the skin and subcutaneous tissue. Muscle and synovial linings are less frequent sites of origin5,6. The natural history of haemangiomas is to enlarge slowly. Their growth may be accelerated with a growth spurt as was found in our case or trauma. They can spontaneously regress. Malignant transformation is rare1.They are usually detected early. Despite intramuscular lesions being concealed, 94% present before the age of 30 7,8. Intramuscular haemangiomas are more common in the lower limbs (42–45%)7,8.The thigh is the most common intramuscular site (17–19%)7,8 as is in our case. Wild et al9 found the quadriceps to be affected in five out of 11 cases of intramuscular haemangioma. Watson et al2 found that 16% of all haemangiomas had more than one site.
Clinically, intramuscular haemangiomas usually present with pain (55%)9 and swelling, contrary to our case, with symptoms usually lasting one to five years (range 0–70 years)7. Haemangiomas may have a purpuric discolouration overlying (from cutaneous extension) the lesion. Superficial dilated veins may also be seen with cutaneous extension. A mass is found in 98% of cases10.The mass may be pulsatile or have a bruit. Contraction of the muscle may increase the size of the lesion as is in our case. The mass is usually moveable transversely but not in the line of the fibres. A history of trauma is uncommon (17%), with tenderness and functional impairment found in about 25%7. Over 90% are misdiagnosed before surgery (this was noted in 1957; advances in investigative techniques may have altered this figure)8. Complications may include a mass (direct pressure) effect, cardiac failure from arteriovenous shunting, and a consumptive coagulopathy (Kasabach-Merritt syndrome).
Calcified phleboliths may be seen on radiographs in 25% of cases9. Magnetic resonance imaging has superseded other investigations, especially before surgery as it is noninvasive, can delineate the extent of the lesion, and can differentiate haemangioma from an invasive malignant process11. Angiography is helpful in delineating whether there may be a vascular feeder that can be embolised12. A group of patients investigated with computed tomography revealed that nine out of 12 lesions were more extensive when explored at surgery13.
Treatment methods have varied in the past and include radiotherapy, open surgical resection, arthroscopic excision, arthroscopic ablation with a holmium, YAG laser, embolisation, and the use of sclerosing agents, cautery and freezing5,14.
A review by McNeill and Ray15 in 1974 of intramuscular haemangioma revealed:
Better outcome if lesion localised
Good results with complete excision
Partial excision resulted in continued symptoms
Limited success if treated non-operatively
Amputation is a last resort
Partial excision is associated with an 18% recurrence rate16 because of the infiltrative growth pattern.
Conclusion
Intramuscular haemangiomas around knee should be kept in mind in case of unexplained stiffness of knee joint. MRI should be done if suspected to prevent diagnostic delay and should be treated by wide local excision if possible to achieve good results.
References
1. Moser RP, Barr MS. Musculoskeletal case of the day. Intramuscular hemangioma of the thigh. AJR Am J Roentgenol 1994;162:1465–6.
2. Watson WL, McCarthy WD. Blood and lymph vessel tumors: a report of 1056 cases. Surg Gynecol Obstet 1940;71:569.
3.Brown RA, Crichton K, Malouf GM. Intramuscular haemangioma of the thigh in a basketball Player.Br J Sports Med 2004;38:346–348. doi: 10.1136/bjsm.2003.004671.
4.Winzenberg T, Ma D, Taplin P, Parker A, Jones G: Synovial hemangioma of the knee: a case report. Clin Rheumatol 2006, 25:753-755.
5. Akgün I, Kesmezacar H, Ögüt T, Dervisoglu S: Intra-articular hemangioma of the knee. Arthroscopy 2003, 19:17.
6. Durieux S, Brugieres P, Voisin MC, Goutallier D, Larget-Piet B, Chevalier X: Radiologic vignette. Arthritis & Rheumatism 1995, 38:559-564.
7.Jenkins HP, Delaney PA. Benign angiomatous tumors of skeletal muscles. Surg Gynecol Obstet 1932;55:464–80.
8.Scott JES. Haemangiomata in skeletal muscle. Br J Surg 1957;44:496–501.
9. Wild A, Raab P, Krauspe R. Hemangioma of skeletal muscle. Arch OrthopTrauma Surg 2000;120:139–43.
10. Ferguson IL. Hemangiomata of skeletal muscle. Br J Surg 1972;59:634.
11. Weisberg AL, Haller JO, Wood BP. Radiological case of the month. Hemangioma of the thigh. Am J Dis Child 1989;143:379–80.
12. Murakami M, Nonaka N, Hirata Y, et al. Hemangioma of the temporalis muscle: case report and review of the literature. Surg Neurol 1991;36:388–93.
13. Christenson JT, Gunterberg B. Intramuscular haemangioma of the extremities: is computerized tomography useful? Br J Surg 1985;72:748–50.
14. Schreiner C, Schleberger R: Das synoviale Hämangiom als seltene Differentialdiagnose des juvenilen Hämarthros. Therapie durch Laserablation. Chirurg 1995, 66:1272-1274.
15. McNeill TW, Ray RD. Hemangioma of the extremities. Clin Orthop 1974;101:154–66.
16. Allen PW, Enzinger FM. Hemangioma of skeletal muscle: an analysis of 89 cases. Cancer 1972;29:8.
| How to Cite: Wani IH, Farooq M, Budoo AR. Intramuscular Haemangioma of Vastus Lateralis Presenting as Stiffness of Knee in an Adolescent. Journal of Orthopaedic and Rehabilitation 2015 Jult-Sep; 1(2): 25-27 |
[Full Text HTML] [Full Text PDF]